
Dupuytren’s Disease & Contracture
Dupuytren’s disease presents as a lump (nodule) in the palm of your hand which becomes larger and resembles a cord over time. The lump is often painless but occasionally may become tender and cause a degree of discomfort, which normally resolves over some months, despite the nodule or cord remaining present.
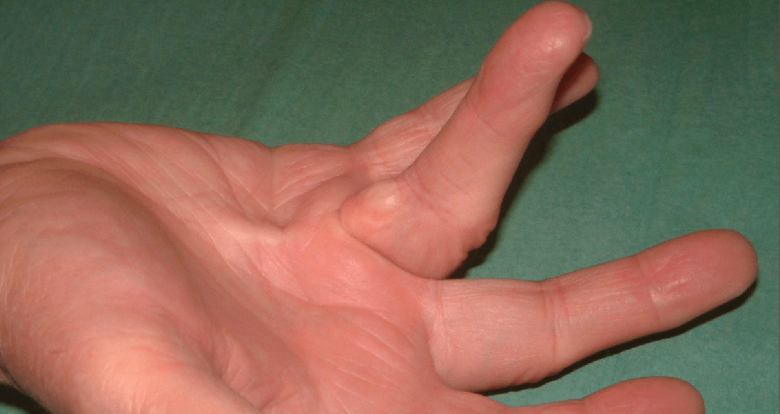
The nodule or cord may subsequently go on to affect one or more fingers, causing them to bend up (contracture). When mild the contracture usually causes no functional problems in using your hand, but if the contractures become more severe, hand function is compromised.
Dupuytren’s disease is not infectious or cancerous, and there is no cure for the condition as it is a genetic condition. Nevertheless, it is possible to influence what happens within your palm with regards to the disease. Patients are not compelled to seek treatment for this condition, but opting for treatment may help straighten your finger(s). If you have a mild case of Dupuytern’s, especially if it is not progressive, you are probably best advised to avoid initial treatment. Should the contracture become more significant, collagenase injection, or surgery and expert rehabilitation are usually the best options.
If you can place your hand flat on a tabletop and your palm touches the table, then usually treatment is not worthwhile. Once your palm no longer touches the table, speak with Dr Jarrett about your treatment options.
How is Dupuytren’s disease and Contracture treated?
Early intervention is the most sensible approach before the contracture is too marked, or if it becomes apparent that progression to a level of impaired function is likely. This way, treatment is more likely to achieve the best results possible with less recovery time, less requirement for too complex a rehabilitation regime and fewer complications.
Percutaneous Needle Fasciotomy (PNF)
If you have ever had a blood test, you will realise that the needle must have a sharp tip to puncture your skin. If you look closely at the needle tip, it is in many ways like a tiny knife, and therefore a needle can be used via small holes in the skin of your palm to divide the fibrous cord causing the contracture thereby causing your finger to straighten. It is similar to a tight piece of string under the skin in your palm causing the finger to be bent, and the needle is being used to snip the string to allow the finger to straighten without actually removing the string.
What are the advantages of PNF?
- PNF is undertaken as a day case under local anaesthetic
- Most patients are able to return to work the next day
- Dressings are required for no more than 2 days
Some contractures are harder to treat and if severe, PNF will not get your finger as straight as other treatments may.
As with all treatments for Dupuytren’s Contracture, there is a risk of the contracture returning over time although PNF or other treatments may be repeated in the future.
A relatively new form of treatment for Dupuytren’s Contracture is an injection of a medication called collagenase which contains an enzyme that dissolves the fibrous tissue causing the cord. This injection causes a degree of swelling and bruising of the hand. For approximately one to five days following the injection of the Collagenase (tradename of XIAFLEX), the injected finger(s) are manipulated in the rooms with an injection of local anaesthetic.
The collagenase injection has a quicker recovery time compared to open surgery with less risk and produces nearly as good a contracture for almost as long a period. There are risks of tendon or ligament rupture (very rare), and 1 in 8 patients have a small skin tear during manipulation which is treated by dressings for a few days.
Unfortunately, the health funds do not cover or cover relatively little of the cost of the injection and since May 2021 the company producing the collagenase medication has increased the cost significantly. However, it is still possible to undertake this treatment if desired.
This procedure involves making some incisions in your hand and removing areas of the thickened fascia within the palm or finger(s) to allow the firm fibrous areas to be removed from your hand and your finger(s) to straighten. In some patients with severe contractures or contracture in several fingers, surgery may be the best option. If you want the maximum chance of improvement in contracture for the longest period possible, then surgery may also be the best choice for you.
Surgery is most often carried out under an arm block, or general anaesthetic. A tourniquet is used to reduce bleeding, and the wounds are dressed by a moderately large bandage or plaster splint following the procedure. The risks of surgery include infection (1-2%), stiffness, bruising, nerve injury numbness on the finger (under 1%), and blood vessel injury (rare). Also, recurrence of the Dupuytren’s contracture with time is likely over time.
After Fasciectomy Surgery – Post-Operative Care
The hand must be elevated to prevent swelling for several days following the procedure. Hand therapy is commenced within a small number of days after surgery unless a skin graft is used, in which case hand therapy is delayed for a week. Absorbable sutures are used which do not require removal.
A splint may be required at night time for several months following the operation, and extensive exercises under the control of our specialist hand therapists are required, both to maintain the correction of the contracture and to regain optimal hand function.
The recovery time, rehabilitation time and intensity will be governed by the pre-operative degree of contracture, and the magnitude of surgery undertaken.
